It is a fact that hysteroscopy is gaining more and more territory in intra-uterine pathology, both diagnostically and therapeutically, thus putting the gynecological world in the heart of a veritable transition phase between, on the one hand, the formerly wide spread blind intra-uterine procedures, such as aspiration and curettage; and on the other hand, more sophisticated under-visual-control techniques, or hysteroscopy. This will more likely lead to particular situations hysteroscopists might be faced with, among which, intra uterine omentum incarceration.
This condition schematically consists of a piece of omentum trapped inside the uterine cavity through a previous misdiagnosed perforation. The patient presents with a history of D&C or other intrauterine procedures, and complains of mild chronic pelvic pain. The clinical examination doesn’t show particular signs. The ultrasound scan ideally demonstrates a hyper-echogenic intra uterine image crossing the uterine wall from inside out, with poor Doppler signals. However, incomplete aspects could be demonstrated, consisting of intracavitary echogenic images, partially invading the uterine wall, thus arousing suspicion of trophoblastic disease, placental remnant or neoplasm. In all cases, MRI is the imaging technique of choice, as it demonstrates both the uterine defect and the fat nature of the tissue, thanks to the fat-suppressed T1-weighted images. The gold standard for management consists of laparoscopic repair.
Ideally, this is how diagnosis and management should be addressed. Yet, in most developing countries, MRI is still out of reach for most patients. The presence of an intra uterine formation usually and directly leads to patient counseling in favor of hysteroscopic diagnosis and resection, if not an iterative curettage in some regions, which should be particularly prohibited under such circumstances.
When hysteroscopy is performed, it is very important to be aware of the hysteroscopic features of incarcerated omentum, as this condition is already a contraindication to hysteroscopy, and mostly, to electrosurgery.
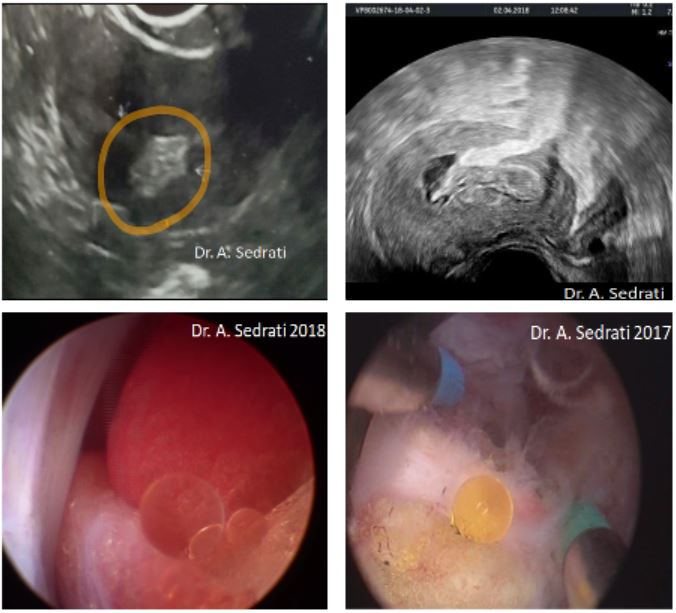
Omentum hysteroscopically appears as an intracavitary yellowish fat like lesion, initially raising the possibility of trophoblast or placental remnants. A case of intramyometrial fat metaplasia has also been reported in the literature, and is thus considered as a differential diagnosis. However, what seems to be pathognomonic of omentum, is that mechanical manipulation of the formation releases yellow drops of lipid nature. This could be termed the “fat drops sign”, or the “Sedrati sign” (fig.7;8), as Dr. Sedrati’s paper was the first in the literature to have described it.
These hysteroscopic findings should lead to increased vigilance and immediate termination of the procedure. Electrosurgery is prohibited. Laparoscopy is to be subsequently scheduled in order to liberate the incarcerated omentum and repair the uterine wall defect.


0 comments on “Hysteroscopic features of intra uterine omentum Incarceration”