Hysteroscopic surgical techniques have advanced to include more endometrial ablation devices, bipolar electrosurgery, hysteroscopic sterilization, and morcellators. As residents complete simulation training programs and learn to become hysteroscopic surgeons, it is important to follow safety tips at each step of the surgery. Hysteroscopy procedures involve the introduction of instruments into the uterus and distention with fluid media. There are particular risks that surgeons must be aware of. The most common perioperative complications associated with operative hysteroscopy are hemorrhage (2.4%), uterine perforation, (1.5%), and cervical laceration. Other complications include fluid overload, visceral injury, infection, air embolism, and rarely death.
The following are a list of safety tips:
1. Appropriate patient preparation involves proper positioning to avoid nerve injury. Care should always be taken since the OR time may be longer than expected.
2. For difficult cases such as Asherman syndrome or large type II submucosal myomas, combined synchronous laparoscopic control or ultrasound guidance may be considered to decrease the risk of perforation and visceral injury.
3. Prior to initiating the surgical procedure, all hysteroscopic equipment should be connected to light sources, suction, and fluid irrigation. It should be tested to ensure it is working appropriately prior to starting the procedure. Backup equipment should be available if technical difficulties occur on the day of surgery.
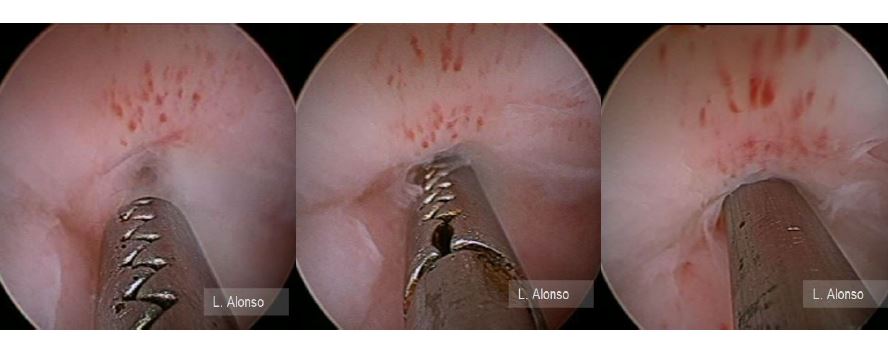
4. During the initial portion of the procedure adequate visualization of the cervix should be obtained. Hysteroscopic dilation of the cervix using the scope and hydrodistension is ideal. If cervical dilation is needed, it is important to only dilate the cervix and not advance the dilator all the way to the fundus to avoid perforation and trauma to the endometrial cavity that will affect visualization. Often in postmenopausal patients, the uterine depth will be small, and perforation could even occur during dilation.
5. In order to avoid air embolism, preventative strategies including flushing air from tubing and making sure that the procedure is stopped and tubing is purged of air when bags are changed. In addition the patient should not be placed in the Trendelenburg position during cervical dilation or during the procedure in order to avoid a suction that may draw air into the uterine cavity. If there is a sudden cardiovascular collapse immediate management should be initiated for an air or CO2 emboli.
6. Care should be taken while inserting the hysteroscope into the uterine cavity to assure that a false tract in the cervical canal has not been made. If one proceeds to close to the depth of sounding without visualization of the cavity this should be considered, with re-attempts to gain entry into the uterine cavity.
7. Hemorrhage may occur during hysteroscopic surgery and can be controlled with electrosurgical coagulation if the bleeding site can be visualized. Other strategies include injection of vasopressin into the cervical stroma or Foley catheter balloon tamponade.
8. Monitor fluid intake to avoid fluid overload. Complications may be prevented by limiting excess fluid absorption, keeping track of ins and outs, and selecting a distending medium such as saline that minimizes risks in healthy patient’s using isotonic solutions. A maximal fluid deficit of 2500 mL is acceptable in a young healthy patient, but is 1000 mL for hypotonic solution such as glycine. The fluid deficit should be limited in older patients or patients with heart failure or renal insufficiency.
9. A preoperative pelvic exam should be completed by the clinician to determine uterine position. Ultrasound guidance may be useful to avoid uterine perforation. If the hysteroscope is inserted and the uterus is unable to be distended at any point during the procedure it is possible there is a uterine perforation. At this point the case should be stopped and reassessed. Laparoscopy may be needed and useful to determine the extent of damage.
10. It is important that if any new devices are used for hysteroscopy that the entire surgical team has been trained and is aware of their use ahead of time. This could include new morcellators or electrosurgical devices.

Please help me More I am from Afghanistan .a country of war and poverty by help of you I hope to learn
LikeLike