Luis Alonso Pacheco / Ana Merino Marquez. Centro Gutenberg. Málaga. Spain
Endometrial polyps are areas of growth of endometrial tissue inside the uterine cavity. They are composed of stroma, glands and blood vessels coated by endometrial lining. Polyps are the most common endometrial pathology found on diagnostic hysteroscopy and represent a frequent cause of operative hysteroscopy.
They are usually benign in nature, although, when symptomatic, about 20% have small areas of hyperplasia being between 0.5% and 1% malignant.
CLASSIFICATION
1-Functional polyps (20%): with similar histologic appearance to normal endometrium with secretory or proliferative changes. They are subdivided into glandular and fibrous, according to the predominant tissue.
2-Hyperplastic (35%): with histologic changes similar to those found in endometrial hyperplasia.
3-Atrophic (44%): with regressive or atrophic changes. These polyps are usually found in menopausal patients.
4-Malignant (1%): with the presence of cancer cells in the polyp.
Endometrial polyps are classified as follows:

There are two concepts that require special attention. The “malignant polyp” and the “pseudo-polyp”. The malignant polyp, a concept first described by Dr F. Coloma, refers to polyps with the presence of malignant cells but the base of the polyp as well as the rest of the uterine cavity are completely normal. The term “pseudo-polyp” refers to thickened areas endometrial polypoid like tissue, less than 1 cm in size that disappears after menstruation because they have no nutritive vessels to support them.
SYMPTOMS
Most polyps are asymptomatic and are usually diagnosed during a routine gynecological examination. If they become symptomatic, usually cause abnormal uterine bleeding, post-coital bleeding, mild pain and sometimes could cause infertility.
EPIDEMIOLOGY
Due to the increase use of transvaginal ultrasound and hysteroscopy in current clinical practice, endometrial polyps are more frequently diagnosed. It is estimated that are present in 1% of asymptomatic women and in about 25% of patients with abnormal uterine bleeding.
DIAGNOSIS
Once the presence of endometrial polyps is suspected, imaging studies are the most sensitive in the diagnosis of intrauterine pathology. Ultrasound is a commonly used imaging modality for the diagnosis of endometrial polyps by direct visualization of the polyp, color Doppler is often used for better visualization of its vascular supply. Often, endometrial polyps are suspected by the presence of increased endometrial thickening. Other techniques that may help in diagnosis are hysterosalpingogram and sonohysterogram. The completion of blind curettage can miss the presence of endometrial polyps in up to 10% of the cases.
The preferred modality for the diagnosis of endometrial polyps is hysteroscopy, in addition to the direct visualization of the polyp; it allows biopsy and even excision at the time of diagnosis.
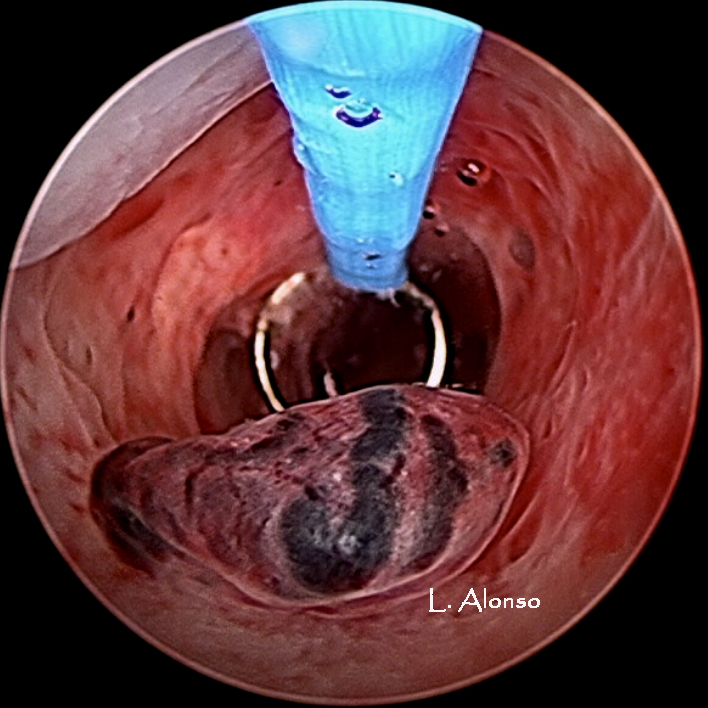
Polyps are seen as areas of growth in the uterine cavity. Generally, they have a spongy surface with striking absence of vascular structures, which differentiates them from submucosal fibroids. They can be single or multiple, pedunculated or sessile, of different size and can be located anywhere in the uterine cavity.
TREATMENT
In general, it is recommended to excise any symptomatic polyp. If the polyps are asymptomatic, it seems appropriate to simply keep an expectant management, with serial ultrasound scans every 6 months to monitor their growth.
The technique for hysteroscopic polypectomy varies depending on the size of the polyp and the available hysteroscope. It is important to emphasize that endometrial polyps are growth areas derived from the endometrium, theydo not invade the myometrium.
1- Mechanical hysteroscopic polypectomy is performed with hysteroscopic scissors or biopsy forceps. This modality is often used for small polyps and can be done in the office setting.
2-Hysteroscopic polypectomy with Versapoint ® bipolar electrosurgery which allows cutting the base of the polyp. It is frequently used in cases of large polyps, they could be fragmented into small pieces facilitating the extraction.
3-Resectoscopic polypectomy: It requires cervical dilation. It is usually reserved for large polyps, often performed in the operating room under general anesthesia.
4-Polyps morcelator: new generation of devices that enable the fragmentation and ease extraction of the polyps.
POSTSURGICAL TIPS
Hysteroscopic polypectomy is a simple technique, which is usually done as an outpatient procedure. The patient may have light vaginal bleeding for several days after surgery, as well as mild discomfort that usually subside with the use of anti-inflammatory drugs (NSAIDs). Most patients return to their daily activities within 24 hours of the procedure.
Hysteroscopy Newsletter

0 comments on “Endometrial Polyps: overview”