Salvatore Giovanni Vitale, M.D. Ph.D
Endometrial polyps represent one of the most common gynecologic pathology frequently causing abnormal uterine bleeding and/or intermenstrual spotting, although the majority of patients with endometrial polyps are asymptomatic. Endometrial polyps are usually benign but the risk for malignancy should be considered when present in postmenopausal women, especially if causing vaginal bleeding. Expectant management is acceptable in some cases, however when symptomatic, large or multiple should be removed. Hysteroscopic polypectomy remains the gold standard modality for the diagnosis and management of the patients with endometrial polyps.
The incidence of surgical complications during hysteroscopic polypectomy is low, making hysteroscopic polypectomy a feasible and safe procedure.
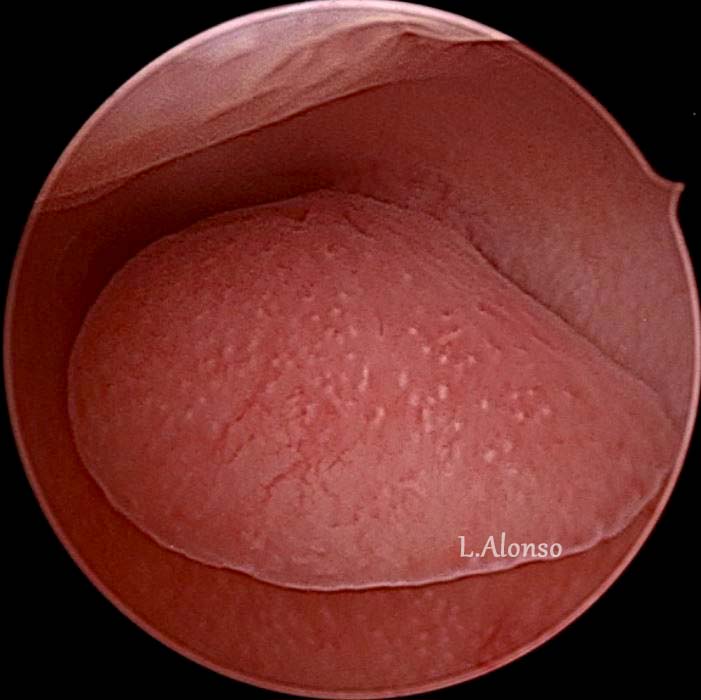
The size of the polyps varies from few millimeters to several centimeters, and their morphology may be sessile with large or small implantation base or pedunculated. They consist of three elements: endometrial glands, stroma, and blood vessels. Known risk factors for the development of endometrial polyps are advanced age (30-50), hypertension, obesity, tamoxifen and hormone replacement therapy use, genetic conditions such as Cowden or Linch syndrome or chromosomal alterations (such as 6 and 20). The risk of developing endometrial polyp increases from menarche to the end of the reproductive age but it is still unclear the de-novo incidence of endometrial polyps during menopause. Endometrial polyps may be asymptomatic, and when causing symptoms, the most common clinical manifestations include abnormal (including postmenopausal, post coital or spotting) uterine bleeding and less commonly infertility.
Rarely polyps of the uterine body, especially of certain volume, trigger in a “reflex way” uterine contractions that displace them progressively towards the cervix, causing at times, their complete expulsion from the cavity with subsequent pain and bleeding.
From a histological point of view we can distinguish hyperplastic, functional, adenomyomatosis with and without atypia, atrophic and pseudopolyps with different clinical therapeutic implications.
Malignant transformation is rare and occurs in 0% to 12.9% of cases. There are several options available for the diagnosis of endometrial polyps.
TRANSVAGINAL ULTRASONOGRAPHY (TVUS)
The primary tool for initial diagnosis of endometrial polyps is transvaginal ultrasonography (TVUS). Endometrial polyps appear as a hyperechogenic lesion with regular contours. Cystic glands may be visible within the polyp. Endometrial polyps are seen as a focal mass or nonspecific thickening of the endomeytrium. These findings, however, are not specific to polyps as leiomyomas (fibroids) particularly submucosal forms may have the same features.
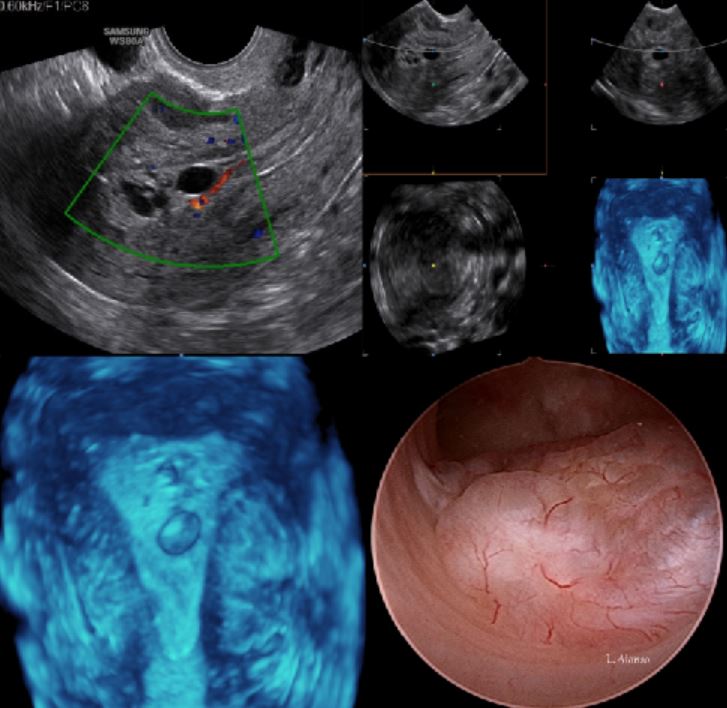
Compared to 2D ultrasonography (TVUS), 3D TVUS with color-flow Doppler has a higher diagnostic accuracy by enhancing endometrial and sub-endometrial vascularization indices; moreover combining endometrial echogenicity, thickness, and volume with 3D TVUS is better than single measurements with 2D TVUS for detecting endometrial polyps.
To obtain the higher diagnostic accuracy, ultrasonographic examination should be carried out during the proliferative phase of a menstrual cycle. Indeed, TVUS has a reported wide sensitivity range from 19% to 96% and a specificity between 53% to 100%, with a positive predictive value (PPV) from 75% to 100%, and negative predictive value (NPV) from 87% to 97% for the diagnosis of endometrial polyps when compared to hysteroscopy and targeted biopsy. A paucity of level I evidence, as well as studies with small sample size, could explain this broad spectrum of data. In a single, large, level II-2 study the reported sensitivity, specificity, PPV, and NPV of TVUS was 86%, 94%, 91% and 90%, respectively.
SALINE INFUSION SONOGRAPHY (SIS) OR SONOHYSTEROGRAPHY (SHG)
Saline infusion sonography (SIS) or Sonohysterography (SHG) is well tolerated by patients and frequently performed when the endometrium on TVUS is abnormal. A small catheter is placed first into the uterine cavity through the cervical canal, and a small amount of normal saline solution is instilled using a syringe into the uterine cavity while performing a TVUS. The normal saline provides a contrast medium, so focal lesions of the endometrium are easily identified. Compared to TVUS alone, saline infusion sonohysterography seems to be little superior to simple TVUS for the diagnosis of intrauterine pathology. Using this technique the polypoid formations are seen as complete mobile intracavitary hyperechoic lesions during fluid injection
HYSTEROSCOPY
Among the diagnostic methods for investigating endometrial disease, hysteroscopy has the highest diagnostic efficacy. Hysteroscopy with guided biopsy represent the gold standard in the diagnosis of endometrial polyps (Figure 4). The main advantage of hysteroscopy is the ability to visualize and remove polyps concurrently.
Diagnostic hysteroscopy alone (without additional biopsies) allows a subjective assessment of the size and characteristic of the lesion with reported sensitivity of 58% to 99%, specificity of 87% to 100%, PPV of 21% to 100%, and NPV of 66% to 99% when compared to hysteroscopy with guided biopsy.
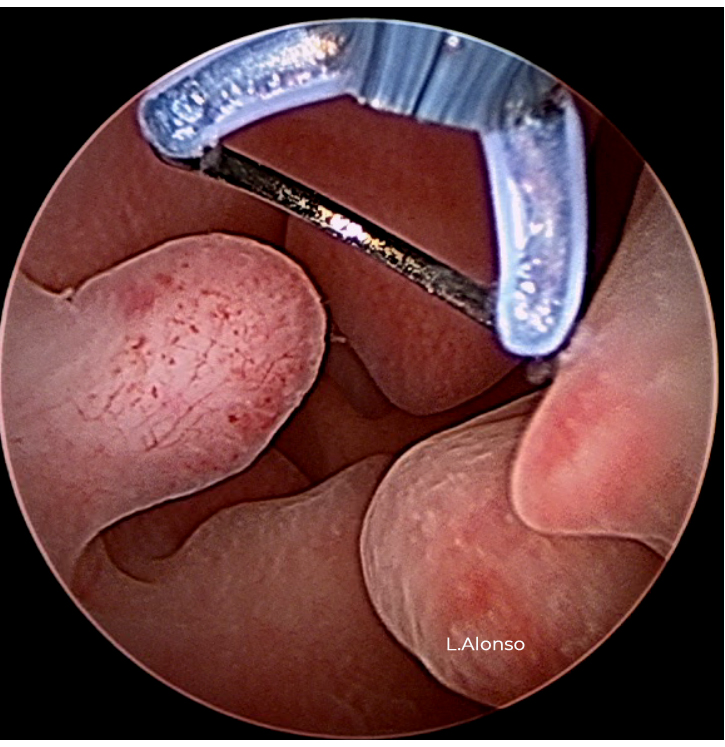
It is important to include in the hysteroscopic evaluation of endometrial polyps some characteristics such as: number, size, location, consistency, vascularization and implant base, all characteristics that can be achieved by the gold standard of hysteroscopy.
MAGNETIC RESONANCE IMAGING (MRI)
Magnetic Resonance Imaging is moderately sensitive to detect endometrial polyps, demonstrating features that are not sensitive but may be specific such as dense fibrous tissue stroma, which reflects a dark T2 fibrous core; thick-walled vascular channels, corresponding to
avid enhancement and endometrial glands, corresponding to intra-tumoral cysts. The predominant T2 signal intensity of polyps has been shown to be similar to the underlying endometrium.
In a retrospective study, which analyzed the characteristics of endometrial polyps in 40 patients undergoing pelvic MRI, the predominant signal intensity on the T2-weighted image (T2WI) was point to hypointense for the underlying endometrium. Hricak et al, in a study analyzing the detection and characterization of endometrial lesions on MRI, showed signal intensity indistinguishable from normal hyperintense endometrium on T2WI in 7 of the 7 endometrial polyps. Another key feature is size, as polyps smaller than 5 mm can be very difficult to distinguish from the adjacent endometrium. So, MRI is not typically obtained to evaluate endometrial polyps.


0 comments on “Evaluation of the uterine cavity and diagnosis of endometrial polyps”